Key messages
- Measles is an urgent notifiable condition that must be notified by medical practitioners and pathology services immediately upon suspicion to the Department of Health.
- Measles is a highly infectious viral illness that can cause serious complications, such as pneumonia and encephalitis.
- Measles is vaccine-preventable, as a part of the MMR (measles–mumps–rubella) vaccine.
- Measles is no longer endemic in Australia, but cases still occur due to importation by overseas travellers.
- People suspected to have measles should be isolated away from others and assessed under airborne precautions while in healthcare facilities.
- Cases should self-isolate until they are no longer infectious.
- Contacts should monitor for symptoms and may be recommended post-exposure prophylaxis.
- Primary school and childcare exclusions apply for cases and unimmunised contacts.
Notification requirement for measles
Measles is an 'urgent' notifiable condition. Measles must be notified upon initial diagnosis (suspected or confirmed) by medical practitioners and pathology services immediately to the Department of Health by calling 1300 651 160 (24/7) and connecting to the relevant Local Public Health Unit. Pathology services must follow up with written notifications within 5 days.
This is a Victorian statutory requirement.
Primary school and children’s services centres exclusion for measles
Children with measles must not attend primary school and children’s service centres from symptom onset until at least 4 days after the onset of rash.
Exclusion requirements for contacts:
- Unimmunised contacts must not attend primary school and children’s service centres for at least 14 days after the onset of rash in the last case of measles. However, they may return if:
- vaccinated within 3 days (72 hours) after exposure; OR
- they receive immunoglobulin within 6 days (144 hours) after exposure.
- Immunised contacts do not need exclusion.
For more information, see the School exclusion table.
Infectious agent of measles
Measles is caused by the measles virus, a member of the genus Morbillivirus in the Paramyxoviridae family.
Identification of measles
Clinical features
Clinical features of measles include prodromal fever, a severe cough, conjunctivitis, and coryza in a moderately unwell child or adult. Koplik spots may be seen on the buccal mucosa. Prodromal symptoms usually last 2 to 4 days.
The most important clinical predictors are included in the clinical case definition for measles, which is an illness characterised by:
- generalised maculopapular rash, usually lasting 3 or more days, and
- fever (at least 38 °C if measured) present at the time of rash onset, and
- cough or coryza or conjunctivitis or Koplik spots.
The characteristic rash appears 2 to 7 days after the onset of the prodrome. It begins on the face before becoming generalised and usually lasts 4 to 7 days. Measles infection (confirmed virologically) may rarely occur without a rash.
Other symptoms can include anorexia, diarrhoea (especially in infants) and generalised lymphadenopathy. People who have been previously immunised may develop attenuated infection with mild or non-classical clinical features, although this is uncommon.
People who are immunocompromised, young children aged below 5 years, pregnant women and adults 20 years of age and older are at increased risk of complications from measles. Complications can include otitis media, pneumonia and encephalitis, which occurs in about one in every 1,000 infected people. Measles infection during pregnancy is associated with an increased risk of miscarriage, premature labour and low birth weight infants.
Subacute sclerosing panencephalitis (SSPE) is an extremely rare and delayed complication of measles, occurring in about one per 100,000 cases. SSPE usually begins about 7 years after the measles infection. It is characterised by progressive inflammation and degeneration of the brain and is always fatal.
Management of suspected cases
People with symptoms of measles are advised to seek medical care, call ahead to the doctor or health facility and wear a mask when leaving the home. On arrival to the health facility, they should be identified and immediately diverted to a separate room for assessment under airborne precautions.
Suspected cases should isolate at home until they’ve been advised whether or not they are a confirmed case of measles. Suspected cases should not go to work, school or public places (e.g. supermarkets).
Diagnosis
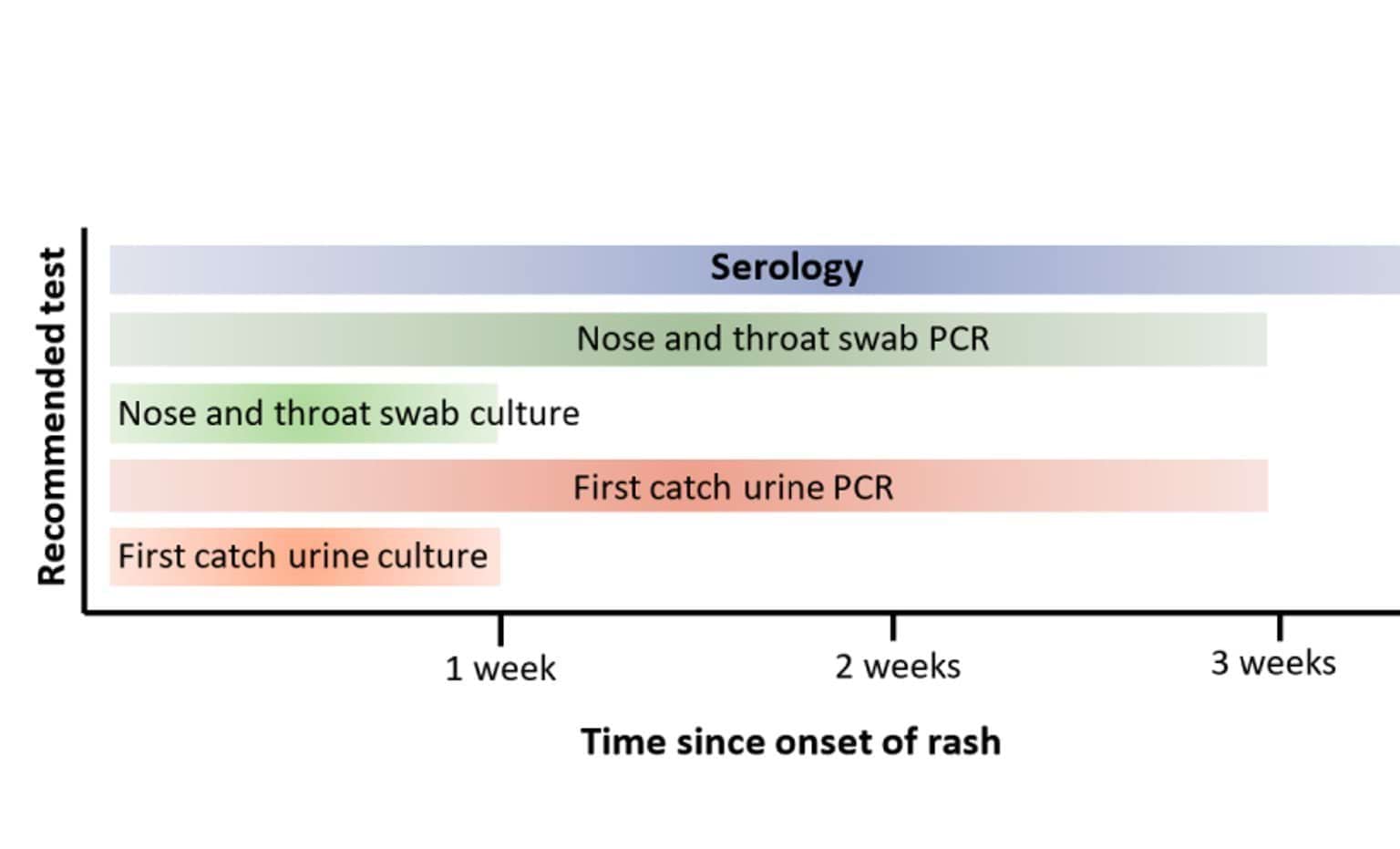
Local Public Health Units (LPHUs) can provide advice on recommended testing for measles at the point of notification of suspected cases by medical practitioners which can include:
- serology (demonstration of measles IgM antibody)
- detection of measles RNA by polymerase chain reaction (PCR) techniques on a nose and throat swab or first catch urine sample. PCR testing for measles is undertaken at the Victorian Infectious Diseases Reference Laboratory (VIDRL)
- viral culture.
Clinicians should test for measles via polymerase chain reaction (PCR) and serology in any patients with compatible symptoms. Label PCR samples as ‘urgent’ and send to VIDRL via your primary pathology provider.
If measles IgM antibody testing is negative on a sample collected 3 days or less after rash onset, it should be repeated 4 to 14 days after rash onset. LPHUs will advise on whether repeat testing is indicated. The diagnosis can also be confirmed by demonstration of a fourfold or greater change in measles IgG antibody titre between acute and convalescent phase sera.
Results of testing should be interpreted in the context of clinical and epidemiological findings, including vaccination history.
Viral genotyping or establishing an epidemiological link to a confirmed case may help to confirm a suspected case.
Public Health Laboratory Network (PHLN) provides information on the laboratory diagnoses of measles.
Incubation period of measles
The incubation period is approximately 10 days but varies from 7 to 18 days from exposure to the onset of fever. It is usually 14 days until the rash appears.
The incubation period can be longer if immunoglobulin is given early in the incubation period.
Reservoir of measles virus
Humans.
Mode of transmission of measles virus
Measles is mainly transmitted by airborne droplets and direct contact with respiratory secretions and contaminated surfaces and objects.
The virus can survive in the environment for up to 2 hours, allowing for transmission in the absence of direct contact with an infectious case. Transmission has been reported in people whose only apparent source of infection was a room previously occupied by a patient with measles.
Period of communicability of measles
Cases are infectious 24 hours prior to the onset of prodromal symptoms until 4 days after the onset of the rash. Where the prodrome is undefined, the onset of the infectious period should be considered to be 4 days before the onset of the rash.
Susceptibility and resistance to measles
People are at increased risk of measles infection following exposure if they are not fully immunised or do not have immunity from previous measles infection.
People who are immunocompromised may still be susceptible to measles even if they have been fully immunised or have had previous measles infection.
Vaccination with 2 doses of a measles-containing vaccine is recommended to protect against measles. The first dose of measles-containing vaccine given at 12 months of age produces protective antibodies in approximately 95 per cent of infants and the second dose given at 18 months of age increases protection to approximately 99 per cent of infants.
Natural infection provides lifelong immunity. Evidence of previous measles infection can be confirmed on prior diagnostic laboratory testing or through serological testing. Self-reported history of measles infection is often unreliable. Therefore serological confirmation is recommended before deferring vaccination based on presumed past infection, as most clinically reported cases subsequently test negative.
Public health significance and occurrence of measles
Globally, the introduction of measles-containing vaccines in infant immunisation programs has led to a significant reduction in measles cases, associated morbidity and deaths. In addition to providing direct protection to the vaccine recipient, immunisation against measles results in the indirect protection of unimmunised people (herd immunity) if high enough coverage is achieved in the population.
Vaccination has several major effects on measles epidemiology, including an increase of the mean age of infection and an increase in the time between epidemics.
Endemic transmission of measles ceased in Australia by the late 1990s as a result of the two-dose vaccination schedule and widespread vaccination. In 2014 the World Health Organization verified that Australia had achieved elimination status for measles, defined as the absence of endemic transmission in a defined geographical area for ≥ 12months.
Although measles is no longer endemic in Australia, there continues to be imported cases in overseas visitors and returning residents, with occasional onwards local transmission.
Interruptions to global vaccination programs during the COVID-19 pandemic, and the resumption of international travel post-pandemic, have led to an increase in measles cases worldwide, heightening the risk of importation to Australia.
Control measures for measles
Preventive measures
Measles-containing vaccines are live attenuated vaccines. All people born during or after 1966 are recommended to receive 2 documented doses of a measles-containing vaccine, unless specific contraindications to live vaccines exist. The measles-mumps-rubella (MMR) vaccine provides safe and effective protection against measles.
Immunisation
The MMR vaccine is free through the National Immunisation Program (NIP) and the Victorian Government funded program:
National Immunisation Program
- infants aged 12 months (MMR) and 18 months (MMRV - measles, mumps, rubella and varicella)
- catch-up vaccination for people up to and including 19 years, and refugees and humanitarian entrants of any age
- refer to the Australian Immunisation Handbook for recommendations for adults
- eligibility for free vaccines under the NIP is linked to eligibility for Medicare benefits.
Victorian Government funded program
- infants from 6 months and before 11 months of age prior to overseas travel. This dose is in addition to the scheduled MMR vaccine doses recommended at ages 12 (MMR) and 18 months (MMRV) under the NIP
- all people born during or after 1966 without documented evidence of receipt of 2 valid doses of measles containing vaccine or without serological evidence of immunity
- includes people not eligible for Medicare.
Immunisation providers should ensure on-time childhood MMR vaccination at 12 months and 18 months, and check and offer MMR vaccination to anyone who does not have evidence of 2 valid doses of measles-containing vaccine or serological immunity.
Refer to the NCIRS clinical decision tool to support measles immunisation.
Serological testing for immunity to measles is not routinely recommended before or after routine administration of the 2-dose schedule. People (with the exception of pregnant women and immunocompromised people) can receive MMR vaccine without serological testing. This is important in the context of a local outbreak, as well as pre-travel situations to maximise opportunities for vaccination.
Pregnant women
Measles-containing vaccines are contraindicated in pregnant women. Vaccination should be deferred until postpartum. Breastfeeding women can receive the MMR vaccine. Vaccinated women should avoid pregnancy for 28 days following vaccination.
People who are immunocompromised
Measles-containing vaccines are contraindicated in people who are immunocompromised. This includes people who are significantly immunocompromised because of a medical condition or receiving high-dose immunosuppressive therapy.
Healthcare workers
Unimmunised healthcare workers, including medical practice staff, born during or after 1966 are at high risk of measles infection. The measles vaccination status of all healthcare workers should be assessed before they commence work, and non-immune workers should be vaccinated with 2 doses of MMR vaccine.
For further guidance refer to the Australian immunisation Handbook - Measles.
How to access the vaccine
MMR vaccine is widely available through GPs, community pharmacies, Aboriginal Health Services and local councils.
Immunisation providers can order MMR vaccine through their government vaccine account via Onelink online.
Control of case
There is no specific treatment for measles. Treatment is supportive or aimed at managing complications of measles.
When seeking medical care, suspected or confirmed cases of measles should call ahead to the doctor or health facility and wear a mask when leaving the home. On arrival to the health facility, they should be identified and immediately diverted to a separate room for assessment under airborne precautions.
If unable to put in respiratory isolation, the case should be managed in a single room with a closed door. Cases who are hospitalised should be isolated and cared for under airborne precautions, ideally in a room with negative pressure ventilation, until they are no longer infectious.
People with measles should isolate at home until they are no longer infectious, usually until 4 days after the onset of rash. In particular, they should avoid contact with people who have an increased risk of severe illness, such as people who are immunocompromised, young children and pregnant women. Cases should not go to work, school or attend public places (e.g. supermarkets).
Children with measles must be excluded from primary school and children’s services until at least 4 days after the onset of rash.
LPHUs investigate all suspected cases of measles to confirm the diagnosis and follow up confirmed cases to investigate the source of infection, identify other cases, identify and protect susceptible contacts, and prevent onward transmission in the community.
Control of contacts
People who have been exposed to measles are at increased risk of infection and may be designated as contacts. Contacts are notified of their exposure, advised to monitor for symptoms, and advised on protective measures. Susceptible contacts may be recommended to receive post-exposure prophylaxis (PEP).
LPHUs will trace and manage susceptible community contacts of cases. Identifying and protecting susceptible contacts exposed in healthcare institutions, such as medical practices or emergency departments, is the responsibility of the individual institution.
Contacts include (in priority order for prophylaxis):
- All household members, and other settings where people share communal facilities (for example, hospital, boarding schools, military barracks).
- All children and adults in family day care, childcare, preschool, school or other educational settings who share a classroom with the case.
- People who stayed in a waiting area at the same time as the case (for example, patients in a healthcare facility’s waiting room and any people accompanying those patients) and people who waited in the waiting area or who were seen in the same consultation room up to 30 minutes after the case left.
- All work colleagues of the case who share the same work area or communal facilities.
- Others who attend or work in the same educational institution as the case, and may have spent time in the vicinity of the case, but do not share a classroom (for example, in a high school, college or lecture theatre block).
- Passengers on an aeroplane.
Contacts who cannot be individually identified but who may have been present in the general area where the case was known to be (for example, in cinemas, shopping centres, aircraft, airport transit lounges, trains and restaurants) may be notified of their exposure through public messaging, media or other communication.
A person considered susceptible to measles is someone who cannot provide acceptable presumptive evidence of immunity to measles. A person can be considered to have acceptable presumptive evidence of immunity to measles if they meet one of the following criteria:
- people born during or after 1966 who have documented evidence of receiving 2 doses of a measles-containing vaccine with both doses given at ≥ 12 months of age and at least 4 weeks apart (unless serological evidence indicates otherwise)
- people born before 1966 (unless serological evidence indicates otherwise)
- documented evidence of immunity (a detectable measles-specific IgG)
- documented laboratory definitive evidence of prior measles.
Primary school and childcare exclusions apply for unimmunised contacts (see above).
Post-exposure prophylaxis
Susceptible contacts should be provided with either MMR vaccine or normal human immunoglobulin (NHIG) according to:
- time elapsed since exposure to an infectious case (where there has been ongoing exposure, such as with household contacts, the time since exposure should be calculated from the first contact during the infectious period)
- age
- previous MMR vaccination history
- current pregnancy or immunosuppression.
In general, measles-containing vaccine is recommended as PEP within 3 days (72 hours) from first exposure to an infectious case of measles.
In general, NHIG is recommended as PEP within 6 days (144 hours) from first exposure to an infectious case of measles and is usually reserved for contacts at higher risk of infection or severe illness such as:
- susceptible household contacts (outside of the MMR PEP window)
- immunocompromised individuals
- pregnant women
- infants who are too young to be vaccinated.
People who receive NHIG for measles PEP will not be able to receive MMR or MMRV vaccine for at least 5 months. Children may need to have their vaccinations adjusted as per the National Immunisation Program Schedule.
For further information on PEP refer to the Communicable Diseases Network Australia (CDNA) Measles National Guidelines for Public Health Units.
For further information on MMR vaccine or NHIG refer to the Australian immunisation Handbook - Measles.
Immunoglobulin prophylaxis
The recommended dose of NHIG is 0.2 mL/kg body weight (maximum dose = 15 mL) given by deep intramuscular injection. Pregnant women and eligible immunocompetent children receive this dose. Children and adults who have immunodeficiency diseases such as leukaemia, lymphoma or HIV infection require a higher dose (0.5 mL/kg body weight, maximum dose = 15 mL).
Infants 5 months and under are now recommended to receive NHIG regardless of the birth mother’s immunity to measles.
Control of environment
Any room visited by a case while they are infectious should be left vacant for at least 30 minutes after the patient has left. The latter period is based on the recognition that normal room ventilation systems ensure that levels of airborne viruses and virus survival diminish rapidly. This includes medical consulting rooms. Environmental clean-up is not generally recommended, although items contaminated with nasal and throat discharges should be disposed of carefully.
Outbreak measures for measles
Outbreaks in the community occur sporadically as a result of imported measles cases exposing local susceptible people. The epidemiology of outbreaks has changed with the introduction of childhood vaccination, and young adults are now at highest risk. Outbreaks in schools may still occur if there are significant numbers of unvaccinated students.
Outbreak control relies on early diagnosis and notification of cases, prompt isolation of infectious cases, and timely and effective identification of contacts, with provision of advice and PEP and/or quarantine, as appropriate. In defined groups of susceptible people, where exposure has occurred but it is too late or not feasible to identify individuals for whom PEP may prevent infection, widespread vaccination may be indicated to minimise ongoing transmission within the group.
LPHUs alongside the Department of Health conduct detailed investigations of outbreaks.
Special settings
Schools and childcare
Although outbreaks mainly affect unvaccinated children, highly vaccinated school or childcare populations have also been affected.
Cases are excluded from school and childcare for at least 4 days after rash onset.
Immunised contacts are not excluded. Unimmunised/non-immune contacts should be excluded until 14 days after the first day of appearance of the rash in the last case.
If unimmunised contacts are vaccinated within 72 hours of their first contact with the first case or if they receive immunoglobulin within 144 hours of the contact, they may return to school.
During an outbreak, children and their siblings who are aged from one year to 18 months should receive their routine second dose of measles-containing vaccine early (but not less than 4 weeks after their first dose).
Measles resources
Health professionals
Measles contact information - Information for contacts of a measles case.
- Social tile 1080x1080 - Exposed to measles travelling overseas?
- Social tile 1080x1080 - Measles vaccine offered here
- Social tile 1080x1080 - Travelling overseas? (Measles vaccine)
Community resources
- Social tile 1080x1080 - General (measles)
- Social tile 1080x1080 - Measles symptoms
- Social tile 1080x1080 - Check measles vaccination status
- Social tile 1080x1080 - Measles testing
- Social tile 1080x1080 - Get vaccinated (measles)
- Social tile 1080x1080 - Catch-up vaccinations (measles)
- Social tile 1080x1080 - Travel vaccinations (measles)
Translated resources
Updated